Breast health rarely announces itself loudly. It whispers. A slight discomfort. A small lump. A change that feels easy to ignore for “just a few more days.”
In clinical practice, what stands out is not a lack of awareness but a pattern of delayed decisions shaped by assumptions. Many women do the right things eventually, but often later than ideal, not because they didn’t care, but because they misunderstood what their body was trying to signal.
Over time, these patterns form a quiet list of mistakes. Not careless mistakes, but human ones. And correcting them early can make the difference between simple reassurance and complex treatment.
1. Normalising Persistent Breast Pain Without Understanding It
Breast pain is often brushed aside as hormonal, especially when it appears around the menstrual cycle. While this is frequently true, not all pain follows predictable patterns.
Pain that is localised, persistent, or unrelated to cycles deserves attention. In practice, many patients who come in for what they thought was “routine discomfort” are often dealing with cysts, inflammation, or structural changes that could have been addressed earlier.
The issue is not the pain itself. It is the assumption attached to it.
2. Reacting Emotionally to Lumps Instead of Clinically
A breast lump carries emotional weight. For some, it triggers immediate panic. For others, it triggers denial. Clinically, the reality is more balanced. A significant number of breast lumps are benign, especially in younger age groups. Conditions like fibroadenoma are common and manageable. However, without proper evaluation, no lump can be confidently categorised.
What often complicates cases is delay, either due to fear or overconfidence. Both lead to the same outcome: uncertainty that lingers longer than it should.
3. Waiting for “More Symptoms” Before Consulting
A common internal dialogue goes something like: “Let me wait and see if anything else happens.” The problem is that breast conditions do not always evolve dramatically in the early stages. Many remain subtle, stable, and easy to overlook.
Early consultation does not mean immediate intervention. In many cases, it simply means structured observation with medical clarity, which is far more reassuring than guesswork.
4. Misunderstanding Fibroadenoma and Overcorrecting Decisions
Fibroadenoma sits in a confusing space for many patients. It is benign, yet it involves a lump. It is common, yet unfamiliar.
This leads to two opposite reactions:
✔ Ignoring it completely
✔Opting for surgery too quickly
In reality, management depends on size, growth pattern, symptoms, and patient comfort. Many cases require monitoring, while some benefit from minimally invasive removal.
The key mistake is treating all fibroadenomas the same.
5. Treating Google as a Diagnostic Tool
Search engines are often the first stop after noticing a symptom. While access to information is valuable, it lacks context.
A single symptom can map to multiple conditions, and online content often represents extremes. This creates either unnecessary fear or false reassurance.
In clinical settings, it is common to see patients who arrive with pre-formed conclusions that do not match their actual condition. Correcting this takes time and adds emotional strain.
6. Skipping Structured Self-Awareness
Self-examination is often advised, but rarely practiced consistently or correctly.
The purpose is not to detect disease with certainty, but to build familiarity. When someone knows their baseline, even subtle changes become noticeable. Without this awareness, changes are often detected later or feel more alarming than they actually are.
7. Avoiding Follow-Ups Once Symptoms Reduce
Relief often creates a false sense of completion. If pain reduces or a lump feels unchanged, follow-ups are postponed or skipped.
However, breast health is not always linear. Some conditions require interval monitoring, not because they are dangerous, but because they need to be tracked over time.
Skipping follow-ups removes that safety layer.
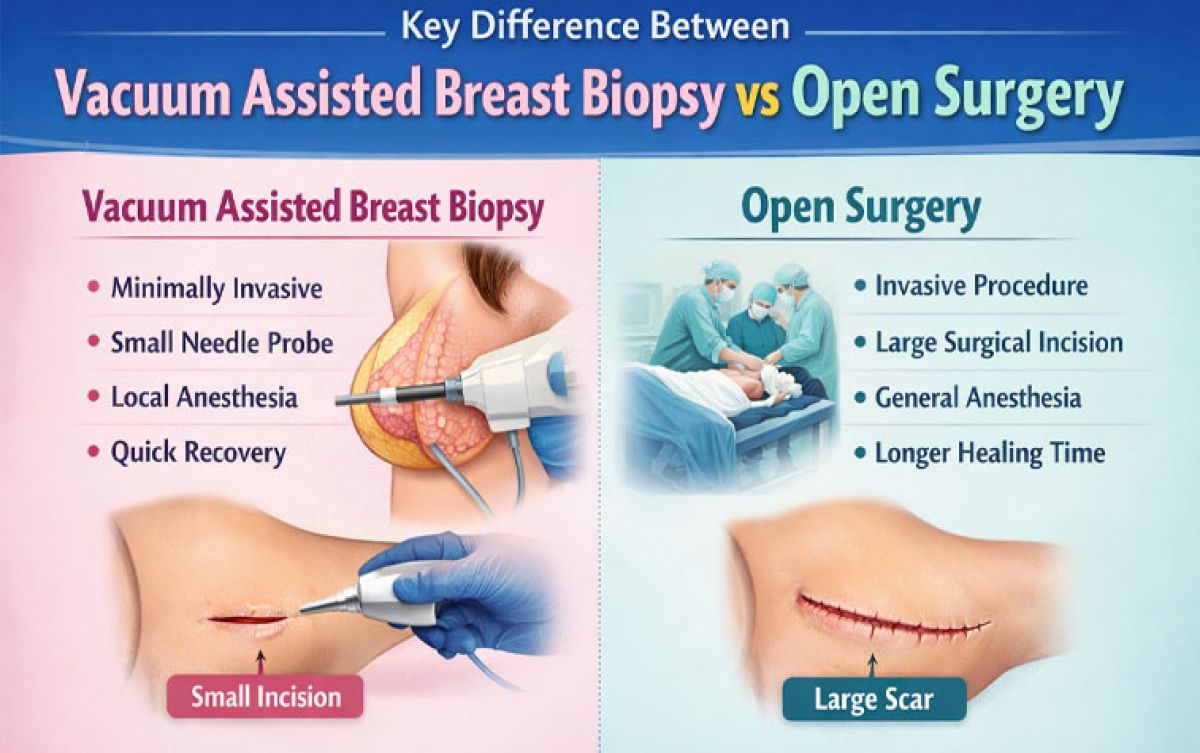
8. Assuming Surgery Is Inevitable
There is a common perception that visiting a specialist will automatically lead to surgery.
In reality, modern breast care is increasingly conservative and evidence-based. Many conditions are managed without surgery, and even when intervention is required, techniques focus on minimal invasion and preservation.
This misconception often delays the first consultation unnecessarily.
9. Letting Discomfort Delay Important Conversations
Breast health is still, in many spaces, a topic discussed in lowered voices. This hesitation delays not just consultation, but even basic conversations with family or primary doctors.
The body, however, does not adjust its signals based on comfort levels. It communicates when something needs attention, regardless of how easy it is to talk about.
10. Believing Age Is a Protective Shield
Younger women often assume that serious breast conditions are unlikely at their age. While risk does increase over time, age does not eliminate possibility.
What changes with age is probability, not certainty. Awareness should remain consistent across all age groups.
Mistakes vs Correct Approach
| Common Mistake | What to Do Instead |
| Ignoring persistent breast pain | Track patterns and consult if pain is unusual or prolonged |
| Panicking or ignoring breast lumps | Get every new lump clinically evaluated |
| Waiting for more symptoms | Seek early consultation for clarity |
| Misunderstanding fibroadenoma | Follow personalised treatment or monitoring plans |
| Relying only on online information | Use it as a guide, not a diagnosis |
| Skipping self-examination | Practice monthly self-awareness |
| Avoiding follow-ups | Stick to the advised monitoring schedules |
| Assuming surgery is necessary | Explore all treatment options first |
| Hesitating to talk about symptoms | Normalise conversations around breast health |
| Believing age eliminates risk | Stay aware at every stage of life |
Where Expertise Changes the Outcome
Breast health is not just about identifying a condition. It is about interpreting it correctly, at the right time, and responding with balance.
This is where experience plays a defining role.
Dr. Rohan Khandelwal in Gurugram, brings a focused practice in breast diseases and surgery, with years of experience dedicated exclusively to this field. His approach combines:
✔ Accurate, evidence-based diagnosis
✔ Clear and structured patient communication
✔ Preference for conservative and breast-preserving techniques
✔ Long-term monitoring and support where needed
At Breast Health, the emphasis is not just on treatment, but on helping patients understand what is happening and why. This clarity often reduces fear more effectively than reassurance alone.
For patients across Gurugram, Delhi NCR, and Haryana, this approach translates into care that is not rushed, not exaggerated, and not delayed, but appropriately timed and thoughtfully delivered.
Frequently Asked Questions
No, breast pain is most often linked to hormonal changes, cysts, or benign conditions rather than cancer. However, if the pain is persistent, localised, or different from your usual pattern, it is important to get it evaluated to rule out any underlying issue.
No, many breast lumps are non-cancerous and commonly include conditions like fibroadenomas or cysts. That said, any new lump should always be examined by a specialist to accurately determine its nature and avoid unnecessary worry or delay.
A breast self-exam should ideally be done once a month, preferably after your menstrual cycle when tenderness is minimal. Regular checks help you understand your normal baseline and make it easier to notice any unusual changes early.
Fibroadenoma is a benign condition and is generally not harmful, but it should not be ignored. Proper diagnosis and periodic monitoring help ensure that it remains stable and does not require intervention.
You should consult a specialist if you notice a lump, persistent pain, nipple discharge, or any visible change in the breast. Early consultation provides clarity and often leads to simpler, more effective management.